What Can You Do About Claim Denial Due To Unbundling?
Unbundling continues to be a top claim denial reason for providers. It may be due to the National Correct Coding Initiative (NCCI) which was implemented in 1996. CMS’ claims payment processing system uses “edits” to identify and reject incorrect combinations of HCPCS procedure codes.
Over 2.5 Million
Practioner PTP Edits
Know what medical procedures can and cannot be billed together by the same physician in the same session in seconds. Medicare and private payers use NCCI to audit your CPT and HCPCS coding – why not use the same tables they use and lower your audit exposure!
Two Low Cost Solutions!
CorrectCoder for EditsPC/Windows application ($179 quarter)
CorrectCoder for Edits
Book ($199)
The National Correct Coding Initiative (NCCI)
Are your claims getting denied for unbundling or incorrect code combinations? It may be due to the National Correct Coding Initiative (NCCI). The NCCI was implemented in 1996 by CMS (formerly HCFA) to identify and eliminate incorrect billing of medical services by looking at all combinations of codes “edits” on a single patient encounter often resulting in a claim denial.
The purpose of the NCCI Procedure-to-Procedure (PTP) edits is to prevent improper payment when incorrect code combinations are reported. The NCCI contains one table of edits for physicians/practitioners and one table of edits for outpatient hospital services. The Column One/Column Two Correct Coding Edits table and the Mutually Exclusive Edits table have been combined into one table and include PTP code pairs that should not be reported together for a number of reasons. The purpose of the NCCI MUE program is to prevent improper payments when services are reported with incorrect units of service.
The National Correct Coding Initiative promotes national correct coding methodologies and reduces improper coding which may result in inappropriate payments of Medicare Part B, Medicaid and private insurance claims.
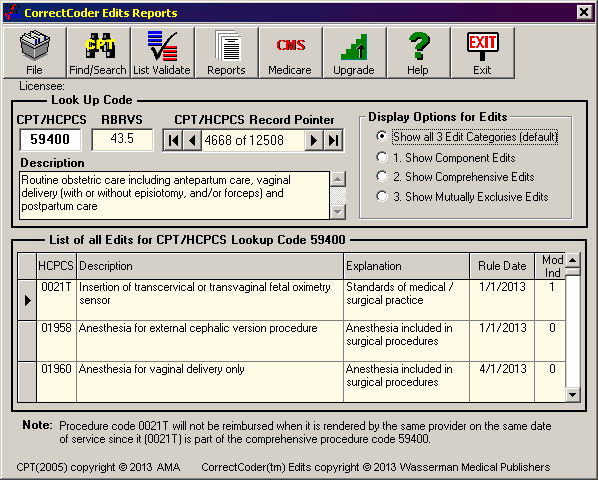
CorrectCoder Main Screen
CorrectCoder for Edits is being used by providers, administrators, private payers, managed care, HMO/PPO/PHO/TPAs, billing services and health care consultants. Over 2.5 million ”edit pairs” (two codes that cannot be billed by the same day by the same physician), and rules for exceptions (modifier -59)
CorrectCoder for Edits simplifies the government’s Correct Coding Initiative (CCI) into one main screen with easy-to-use searches.
See Tour for detailed screeen shots.